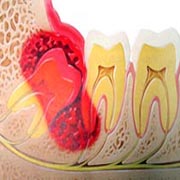
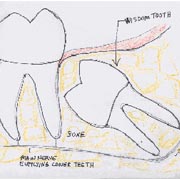
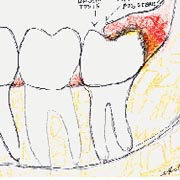
Wisdom teeth also known as third molars are the last teeth to erupt. Wisdom teeth may become a problem for you as they grow and develop in each corner of your mouth. Problems often develop gradually since development normally spans several years. Nevertheless, these gradual changes can cause sudden and severe pain. Understanding why such things can happen may help you to deal with these problems, or better still, to encourage you to take preventive measures before they occur.
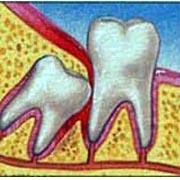
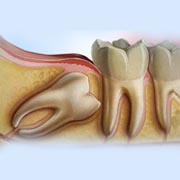
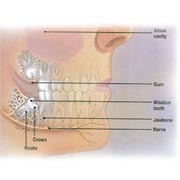
The jawbone grows to approximately its adult size by your late teens. Unfortunately, that size is often too small to hold developing wisdom teeth. This happens because our jaws are smaller than those of early humans who needed large jaws and more teeth for their tougher diet.
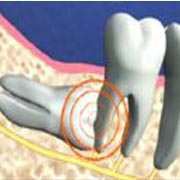
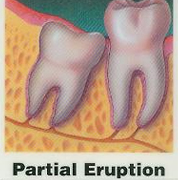
When there is not enough room for your wisdom teeth, they may become impacted, or partially trapped in the jawbone and gums. The crown, or top of the tooth, may erupt, or just break through the gum, or it may remain completely within the bone. The roots can grow in unusual directions and may cause a variety of problems in your mouth and with your sinus cavity or the nerve in your lower jaw. The primary preventive measure for wisdom teeth is removal, preferably at an early stage.
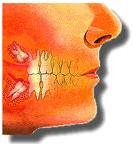
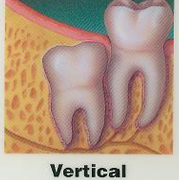
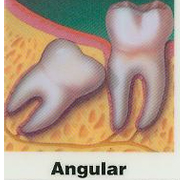
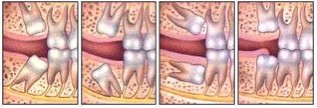
A tooth becomes impacted due to lack of space in the dental arch and its eruption is therefore prevented by gum, bone, another tooth or all three. Lack of space occurs because our jaws have become smaller through evolution. We do not lose teeth through decay as frequently as in the past and our diet does not wear down our teeth as much.
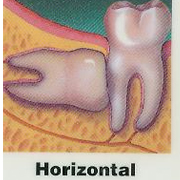
Impacted wisdom teeth can grow in a variety of directions. This is illustrated below.A wisdom tooth may grow toward your other teeth, away from them, or even in horizontal or vertical positions. When such conditions occur, it's far simpler and less painful to have them removed early before they have a chance to firmly anchor in your jaw as the teeth grow and the roots lengthen.
Wisdom teeth generally cause problems when they erupt partially through the gum.
Below are the most common reasons for removing wisdom teeth.
1. Tooth decay
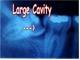
Saliva, bacteria and food particles can collect around an impacted wisdom tooth, causing it, or the next tooth to decay. It is very difficult to remove such decay. Pain and infection will usually follow.
2. Gum infection
When a wisdom tooth is partially erupted, food and bacteria collect under the gum causing a local infection. This may result in bad breath, pain, swelling and the inability to open your mouth fully. The infection can spread to involve the cheek and neck. Once the initial episode occurs, each subsequent attack becomes more frequent and more severe.
3. Pressure pain
Pain may also come from the pressure of the erupting wisdom tooth against other teeth. In some cases this pressure may cause the erosion of these teeth.
4. Orthodontic reasons
Many younger patients have had prolonged orthodontic treatment to straighten teeth. Wisdom teeth may cause movement of teeth particularly the front teeth when they try to erupt. This will compromise the orthodontic result.
5. Prosthetic reasons
Patients who are to have dentures, constructed should have any wisdom tooth removed. If a wisdom tooth erupts beneath a denture it will cause severe irritation and if removed, the patient will need to have a new denture constructed as the shape of the gum will have changed.
6. Cyst formation
A cyst (fluid filled sac) can develop from the soft tissue around an impacted wisdom tooth. Cysts cause bone destruction, jaw expansion and displacement or damage to nearby teeth. The removal of the tooth and cyst is necessary to prevent further bone loss. Tumors may develop within these cysts or the jaw may fracture spontaneously if the cyst grows very large.
Impacted wisdom teeth are almost certain to cause problems if left in place. This is particularly true of the lower wisdom teeth. Such problems may occur suddenly and often at the most inconvenient times.
It is now recommended by dentists that impacted wisdom teeth be removed between the ages of 14 and 22 years whether they are causing problems or not. Surgery is technically easier and patients recover much more quickly when they are younger. What is a relatively minor operation at 20 can become quite difficult in patients over 40. Also the risk of complications increases with age and the healing process is slower.
It may be advisable to have them removed before traveling if you are going to an area where specialist dental services are not readily available and your wisdom teeth are impacted.Should a wisdom tooth be removed when an acute infection is present?
Generally, no. Surgery in the presence of infection can cause infection to spread and become more serious. Firstly, the infection must be controlled by local oral hygiene, antibiotics and sometimes the extraction of the opposing wisdom tooth.
The 'Pros & Cons' of wisdom tooth removal
Wisdom teeth may be hard to access with your toothbrush, or floss. Over time, the accumulation of bacteria, sugars and acids may cause a cavity to form in the tooth. If it is not restored with a filling, the cavity may spread and destroy more tooth structure causing severe consequences to the tooth and surrounding supportive structures.Due to the difficulty of keeping these teeth clean with your daily brushing and flossing, bacteria and food debris remaining on the wisdom teeth may present a foul smell causing bad breath.
A wisdom tooth that is still under the gums in a horizontal position rather than a vertical position may exert pressure on surrounding teeth causing crowding and crooked teeth. This also may occur if there is not enough space in the mouth for the wisdom tooth. This may warrant braces to repair the damage.A wisdom tooth that is still under the gums may become irritated. The gum tissue that lay over the tooth may harbour food debris and bacteria that gets trapped under the gum resulting in an infection in the gums.
There is the potential for more problems to occur the longer you wait and the older you get. This is because as you get older, the bone surrounding the tooth becomes increasingly dense making the tooth more difficult to remove. The healing process may also be slower.
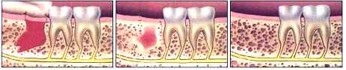
The healing process begins immediately after surgery as your body sends blood to nourish the tooth socket. Simple pressure from a piece of gause is usually all that is needed to control the bleeding and to help a blood clot to form in the socket, which promotes healing. Within a day or two, soft tissue begins to fill in the socket, aided by the blood clot. Eventually, the bone surrounding the socket begins to grow, filling in the socket completely. This is illustrated below.
As your mouth heals, you can promote faster healing and avoid complications by simply following the care instructions that our particiapting dentists will give you. While you may experience some discomfort as your mouth heals, following simple instructions will normally be all that is needed. However, you should call our participating dentists if you experience excessive bleeding or swelling, persistent and severe pain, fever, or any reaction to medications. A follow-up examination may also be scheduled to make sure that the socket is healing properly and that your mouth is returning to a normal, healthy state.
Following the removal of your wisdom teeth it is important that you call our participating dentists if any unusual bleeding, swelling or pain occurs. The first 6-8 hours after the extraction are typically the worst but are manageable.
At first, it may be possible to feel small fragments of bone with your tongue. These are the edges of the tooth socket and will soon disappear as the gum heals. Depending on the type of stitches used, they may need to be removed. Arrangements will be made for this to be done. If dissolvable stitches have been used, they will disappear 7 to 10 days after the operation.
Below are some tips to assist you after the operation.
Disturbing the wound may invite irritation, infection and bleeding. Chew on the opposite side for the first 24 hours.
Smoking will promote bleeding and interfere with healing.
This will promote bleeding and may dislodge the blood clot which could result in a dry socket.
If the area is not closed with stitches, a pressure pack made of folded sterile gauze pads will be placed over the socket. It is important that this pack stay in place to control bleeding and to encourage clot formation. The gauze is usually kept in place for 30 minutes. If the bleeding has not stopped once the original pack is removed, place a new gauze pad over the extraction site.
After surgery, some swelling is to be expected. This can be controlled through the use of cold packs which slow the circulation. A cold pack is usually placed at the site of swelling during the first 24 hours in a cycle of 20 minutes on and 20 minutes off. After the first 24 hours, it is advisable to rinse with warm saltwater every two hours to promote healing (one teaspoon of salt to a glass of warm water). Do not rinse your mouth out during the first 24 hours because this disturbs the blood clots that are part of the healing process.
Anti-inflammatory medication such as Panadol is used to control minor discomfort following oral surgery. Stronger analgesics may be prescribed by the dentist if the patient is in extreme discomfort.
A soft diet may be prescribed for the patient for a few days following surgery. You can gradually return to a normal diet once any jaw stiffness has settled. Very hot drinks and spicy food can increase pain and bleeding and should be avoided until the gum has healed. Also avoid alcohol as alcohol can increase bleeding and delay healing.
Most people do not experience any complications after having their wisdom teeth removed. Nonetheless, you should plan to see our participating dentists approximately one week later to ensure everything is healing well.
